A finger that is “stuck” in a bent position is more than just a cosmetic issue—it’s a significant functional problem that can interfere with everything from shaking a hand to putting your hand in a pocket to putting gloves on. This specific deformity, where the middle joint of the finger is bent downward, and the fingertip is bent back, is known as a Boutonnière Deformity. It can be the frustrating result of a “jamming” injury or the effects of inflammatory arthritis.
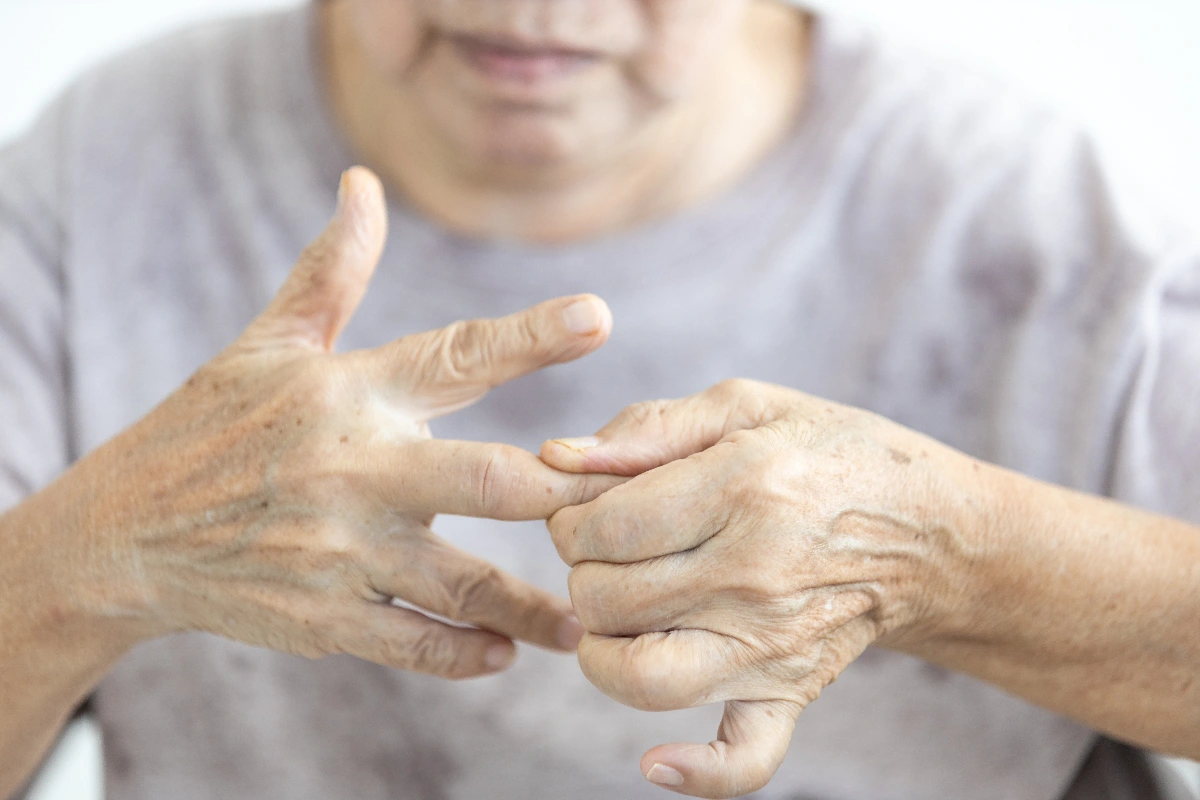
A finger that is “stuck” in a bent position is more than just a cosmetic issue—it’s a significant functional problem that can interfere with everything from shaking a hand to putting your hand in a pocket to putting gloves on. This specific deformity, where the middle joint of the finger is bent downward, and the fingertip is bent back, is known as a Boutonnière Deformity. It can be the frustrating result of a “jamming” injury or the effects of inflammatory arthritis.
Living with this limitation can be a daily challenge, but it does not have to be a permanent condition. Correcting a Boutonnière Deformity requires a complex and delicate reconstructive surgery. As a Harvard-trained specialist in Reconstructive Plastic Surgery and Microsurgery, Dr. Rod French has the expertise to rebalance the intricate structures of your finger and restore a more natural form and function.
The ability to straighten your finger is controlled by a complex, balanced network of tendons called the extensor mechanism. A Boutonnière Deformity occurs when a key part of this mechanism, the “central slip” tendon that attaches to the middle bone of your finger, is torn or stretched.
Without the upward pull of the central slip, the middle joint (the PIP joint) begins to bend downward. This imbalance then causes the other parts of the tendon network to pull the fingertip joint (the DIP joint) backward into hyperextension. The goal of surgery is to reconstruct this delicate tendon mechanism, rebalance the forces across the joints, and restore the finger’s ability to straighten.
It is critically important to fix an acute boutonniere deformity as quickly as possible. If left untreated, the finger at the PIP joint can become permanently flexed rendering later reconstruction of a chronic boutonniere deformity as one of the most difficult surgical reconstructions in all of hand surgery. Early treatment with definitive surgery is paramount.
Surgical repair of the acute injury should be done as soon as possible. Reconstruction can be an option for a persistent, chronic Boutonnière Deformity that interferes with your life. You are likely a candidate if:
A Boutonnière Deformity is a progressive problem. Over time, what starts as a flexible deformity can become a rigid, fixed contracture that is much more difficult to correct. Waiting months or years in the public system for a consultation with a specialist can allow this to happen, potentially leading to a permanent deformity that cannot be fixed even with surgery.
Choosing private care provides timely access to a reconstructive specialist. It allows you to proceed with a corrective surgery while the joint is still supple and the tissues are in the best possible condition for a successful reconstruction. This is a proactive investment in achieving a better, more functional long-term result.
Correcting a Boutonnière Deformity is a complex reconstructive procedure that is tailored to your specific anatomy and the condition of your tendons.
The recovery from a Boutonnière Deformity repair is a long process that requires an absolute partnership between you, your surgeon, and your certified hand therapist.
It is fixed with a complex reconstructive surgery that involves repairing and rebalancing the network of tendons that straighten the finger. The goal is to restore the upward pull on the middle joint.
Yes, in most cases, especially if the joint is still flexible, a surgical reconstruction can significantly improve the deformity and restore the ability to straighten the finger.
Recovery is lengthy and requires commitment. It involves several weeks of initial splinting, followed by several months of intensive, specialized hand therapy to safely regain motion and strength.
This is a complex soft tissue reconstruction. Risks include infection, failure of the repair to heal, and persistent stiffness. The single biggest factor in a successful outcome is strict adherence to the post-operative hand therapy protocol.